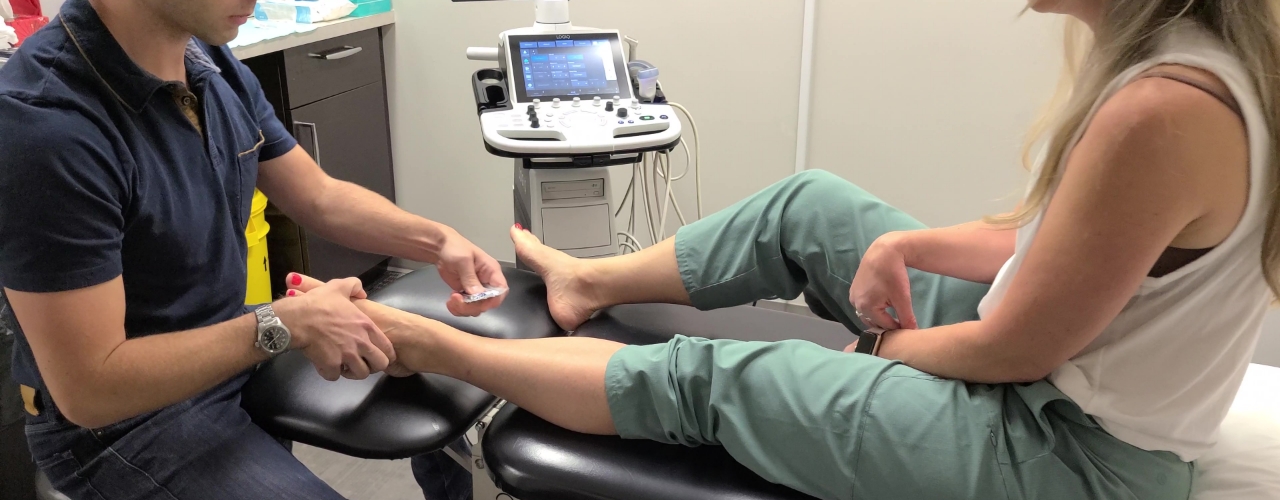
Interventional Pain Management refers to a group of minimally invasive procedures that aim to manage pain, improve function, and quality of life in individuals with chronic pain conditions. Momentum Health offers various interventional pain management procedures such as:
Lumbar Radio Frequency Ablation (RFA)
What is Lumbar Radio Frequency Ablation (RFA)?
This outpatient procedure is used to help with treating lower back, hip and groin pain
What are Lumbar Facet Joints?
Facet joints are found on either side of the spine. Each of these joints is about the size of a thumbnail. In the lumbar spine there are 5 vertebrae that are connected by facet joints.
Facet joints connect vertebrae to one another along with guiding the spine when moving.
Medial branch nerves are located near facet joints. They communicate pain from facet joints. Therefore these nerves tell the brain when the facet joint has been injured or hurt.
Injury to a facet joint typically involves damage to cartilage inside the joint and connecting ligaments surrounding the joint.
Pain from an injured lumbar joint may range from muscle tension to more severe pain. This pain can radiate into different areas, depending on which facet joint is injured/affected.
Do I have Lumbar Facet Joint Pain?
If you have pain for greater than 2 months in the lower back, hip and/or groin area you may have lumbar facet joint pain.
Tests such as X-rays or MRIs do not always show if the facet is the reason for your pain. The best way to test if you have this pain is to block the pain signal from the medial branch nerve.
A Lumbar RFA disrupts the function of the lumbar medial branch nerve. The medial branch nerve is then no longer able to transmit pain signals from the affected facet joint.
RFA Procedure
A thin needle is inserted near the facet joint under fluoroscopy (a type of x-ray). Fluoroscopy is used to position the needle.
With the correct needle position the area will be numbed with anesthetic medication. The Physician will use radiofrequency energy to disrupt the medial branch nerve signal.
How Long Should the Pain Relief Last?
After your Lumbar RFA procedure, you will be monitored for approximately 30 minutes. The clinic will give you appropriate instructions to follow for care after the procedure.
We caution against driving after an RFA procedure.
Post procedure soreness may be experienced. Typically this soreness is caused by muscle and nerve irritation and can last 2 – 4 weeks. The full benefits for pain relief take usually 6-12 weeks.
Nerves will regenerate after the RFA procedure. However the time it takes for them to regenerate varies from 8 – 24 months. Your typical pain may or may not return after this nerve regeneration. If your pain does return, another RFA can be done.
(Please note the RFA procedure is performed at a different location, but follow ups are with Momentum Health)
Ultrasound Guided Percutaneous Needle Tenotomy
What is Ultrasound Guided Tenotomy?
- Tenotomy is a minimally invasive procedure that involves multiple needle passes of the degenerated tendon to disrupt the affected area and induce bleeding from the tendon bony attachment
- This leads to converting the chronic non-healing tendon injury into an acute injury with clot formation and release of healing factors to increase the healing potential
- Tenotomy is performed with a single needle insertion through the skin after administration of a local freezing and under ultrasound guidance with minimal discomfort to the patient
Pre-Tenotomy Recommendations
- Cortisone injections must be avoided in the entire body six weeks prior to Tenotomy and for twelve weeks in the anatomical area that is undergoing Tenotomy
- NSAIDs (Ibuprofen, Advil, Aleve, naproxen, celebrex, diclofenic, Voltaran, etc,) must be avoided two weeks prior to the procedure
- Smoking cessation is strongly recommended as it has been associated with poor tendon healing and recovery
- The use of CBD oil and/or medical marijuana is also recommended to be avoided for two weeks prior to the procedure
Post-Tenotomy Recommendations
- You can expect significantly increased pain for three to seven days after the procedure
- NSAID’s and medical marijuana must be avoided for two weeks after the procedure
- You must immobilize the area that in a brace, air cast, or crutch for a minimum of three days. Lack of immobilization risks rupture of the muscle/ tendon
- Within these three days you should remove the brace three to five times a day to go over range of motion exercises prescribed by your physiotherapist
- After three days you can remove the brace for in-household activities
- If after three days you are required to leave the house for extended periods of time (i.e. to go to work) you must immobilize the joint in the appropriate brace, sling, or crutch until otherwise stated by your physiotherapist
What is Tendinosis?
Tendinosis is a predominately degenerative condition as a result of repetitive stress and tendon failure to adapt and heal. This can be associated with buildup of abnormal calcium in the tendon or tendon tears
Physiotherapy component
- A Physiotherapy Assessment prior to the procedure is to ensure patient education on the post-procedure protective phase and that there are no contraindications
- 8 follow up visits on a weekly interval are to assess recovery and progress with the post-procedure rehabilitation and strengthening protocol
Lumbar Facet Joint Injections
What is a Lumbar Facet Joint Injection?
This outpatient procedure is used to help with diagnosing and/or treating low back, buttock, hip and/or groin pain.
What are Lumbar Facet Joints?
Facet joints are found on either side of the spine. Each of these joints is about the size of a thumbnail. There are typically 5 lumbar vertebrae that are connected by facet joints.
Facet joints connect vertebrae to one another along with guide the spine when moving.
Injury to a lumbar facet joint typically involves damage to cartilage inside the joint and the connecting ligaments surrounding the joint.
Pain from an injured lumbar facet joint may range from mild muscle tension to more severe pain. This pain can radiate into different areas, often buttock, depending on which facet joint is irritated.
Is my pain Lumbar Facet Joint Pain?
If you have pain in the low back, buttock, hip or groin area for greater than 2 months you may have lumbar facet joint pain.
Tests such as X-rays or MRIs do not always show if the facet is the reason for your pain. The best way to test if you have this pain is to block the pain signal from the medial branch nerves which sends the nerve signals from the facet joints to the brain.
The Lumbar Facet Injection Procedure
A thin needle is inserted near the facet joint under fluoroscopy (a type of x-ray). Fluoroscopy is used to position the needle. A small amount of dye is used by the Physician in order to assess if the needle is in the proper position. This can cause some of your symptoms to be reproduced.
With the correct needle position, the facet joint is then injected with a combination of a corticosteroid (anti-inflammatory) and an anesthetic into the irritated facet joint.
(Please note the Lumbar Facet Injection procedure is performed at a different location, but follow ups are with Momentum Health)
How Long Should the Pain Relief Last from a Lumbar Facet Injection?
After your Lumbar Facet Joint Injection, you will be monitored for approximately 15 – 30 minutes. The clinic will give you appropriate directions to follow for care following the procedure.
Post procedure soreness may be experienced. Typically, this soreness is caused by muscle and nerve irritation. You may also notice some numbness and tingling into the leg and foot for a maximum of 4-6 hours.
There should be pain relief immediately lasting 4-6 hours. The corticosteroid takes about 1 week post injection for it to take optimal effects. Pain relief lasts anywhere from a few weeks to several months, depending on the ultimate cause of your facet joint pain.
Important Notes on Lumbar Facet Injection Procedures
Do not stop any anti-platelet/anti-coagulant medications (eg. Aspirin, Plavix, Coumadin, etc.) unless instructed to do so by our physician.
Lumbar Medial Branch Block
What is a Lumbar Medial Branch Block (MBB)?
This outpatient procedure is used to help with diagnosing lower back, hip and groin pain.
What are Medial Branch Nerves?
Medial branch nerves are located near facet joints. They communicate pain from facet joints. Therefore the nerves tell the brain when the facet joint has been irritated or hurt.
Injury to a facet joint typically involves damage to cartilage inside the joint and connecting ligaments surrounding the joint.
Pain from an injured lumbar joint may range from mild muscle tension to more severe pain. This pain can radiate into different areas, depending on which facet joint is irritated.
Medial Branch Block Procedure
A thin needle is inserted near the facet joint under fluoroscopy (a type of x-ray). Fluoroscopy is used to position the needle accurately and safely. A small amount of dye is used by the Physician to assess if the needle is in the proper position. This injected dye can cause some discomfort.
With the correct needle position the area will be numbed with an anesthetic medications.
(Please note the Medial Branch Block procedure is performed at a different location, but follow ups are with Momentum Health)
How Long Should the Pain Relief Last?
After your Lumbar Medial Branch Block procedure you will be monitored for approximately 15 – 30 minutes. The clinic will give you appropriate directions to follow as well as complete a pain diary. This pain diary is very important as it will guide the Physician treatment plan for you.
Pain relief will last for approximately 4-6 hours, until the anesthetic wears off.
Short term pain relief is considered a positive test. The Physician will then determine the next step in your treatment plan.
Post procedure soreness may be experienced. Typically this soreness is caused by muscle and nerve irritation.
Important Notes on Lumbar Medial Branch Blocks
Do not stop any anti-platelet/anti-coagulant medications (eg. Aspirin, Plavix, Coumadin, etc.) unless instructed to do so by the physician.
Please arrive with your pain level 5/10 or greater to ensure that you will be able to notice the effects of the injection. If your pain level is less than 5/10, your injection may be rebooked. You may want to avoid taking pain medications the day of the procedure
Ultrasound Guided Trigger Point Injection
A Combined Physiotherapy & Physician Treatment Program
Ultrasound Guided Trigger Point Injections are designed to optimize the effectiveness of trigger point injections with a combination of exercises, myofascial release, and joint mobilizations. The program will initiate treatment with the idea of establishing ongoing therapy.
Myofascial Pain Syndrome
Most muscle pain centres on sensitive bands in your muscles called trigger points. These trigger points can be painful to the touch and often spread throughout the involved muscle and possibly adjacent muscles.
Muscle pain is very common but people with myofascial pain syndrome have painful muscles that persist or worsen with time.
Treatment for myofascial pain syndrome often requires a combination of physiotherapy, trigger point injections and/or medications.
The Trigger Point Injection Procedure
Trigger point injections involve a medical doctor inserting a needle into a trigger point in your muscle. Trigger point injections may relieve the tension in your muscle originating from the sensitive bands. A small amount of a numbing medication, such as an anesthetic, may be injected into the trigger point each time the needle is inserted.
Myofascial Release is the use of a therapist’s hands to evaluate the texture, tightness and movement of muscles, fascia, tendons, ligaments and nerves. The abnormal tissues are treated using a combination of precisely directed tension with very specific patient movements
Conditions that May Benefit from Trigger Point Injections
- Myofascial Pain Syndrome
- Fibromyalgia
- Muscle Pain and Stiffness
- Muscle Spasms
- Chronic Back Pain
- Chronic Neck Pain
Appointment Guidelines for receiving Trigger Point Injections
Appointment 1
Physiotherapy assessment which includes functional movement screen, evaluation of muscle quality, and joint movement followed by an exercise prescription.
Appointments 2-4
Weekly trigger point injections under ultrasound guidance with a physician followed by physiotherapy
Appointment 5
Re-Assessment two weeks after the last injection, discussion of further treatment plan and exercise progression
Regenerative Injection Therapies may also be recommended
Please call us for more information on these or any of our procedures.
Interventional Pain Management is currently provided by Dr. Abdel Rahman Aly at Momentum Health West Springs.
Your Next Steps…
Book An Appointment
Determine Coverage
Get An Assessment
Start Treatment